1Biomedical Engineering Department, Royal Medical Services,Bahrain
2Department of Radiology, Bahrain Defence Forces Hospital, RCSI-MUB, Bahrain
3Albalqa Applied University , Jordan
Corresponding author email: leena.albalooshi@rms.bh
Article Publishing History
Received:
Accepted After Revision:
This review aims to examine the biological effects of Magnetic Resonance Imaging (MRI) exposure in healthcare professionals working with high-field MRI systems (1.5 Tesla and above). By synthesizing current evidence, it seeks to inform future safety guidelines and highlight potential risks associated with cumulative, long-term exposure among MRI technicians and radiologists. A systematic literature search was conducted on studies published from 2000 to 2024. Databases (e.g., PubMed, Scopus) were queried using key terms such as “MRI exposure,” “occupational health,” and “high-field MRI.” Studies were evaluated based on methodological rigor, relevance to occupational settings, and reported biological effects. The search aimed to identify both short-term and long-term physiological impacts of repeated MRI exposure. Although short-term MRI exposure is generally safe, healthcare workers consistently operating high-field MRI systems may experience transient sensory disturbances (e.g., vertigo, nausea) and possible long-term physiological effects. Findings suggest an elevated concern for cumulative exposure, yet conclusive evidence on the magnitude and nature of these risks remains limited due to variability in study designs and outcomes. While MRI technology plays a pivotal role in diagnostic medicine, ongoing research is needed to clarify the occupational hazards for healthcare professionals exposed to high-field environments. Improved monitoring, standardized safety protocols, and comprehensive longitudinal studies are recommended to ensure the continued safe use of MRI in clinical settings.
electromagnetic fields; Magnetic Resonance Imaging; MRI safety.
Alseddiqi M, Alomran B, Almofleh A, Albalooshi L, Najam O. Effects of Exposure to Magnetic Fields in MRI: A Review of Current Evidence and Future Directions. International Journal of Biomedical Research Science (IJBRS). 2026;02(1)
Alseddiqi M, Alomran B, Almofleh A, Albalooshi L, Najam O. Effects of Exposure to Magnetic Fields in MRI: A Review of Current Evidence and Future Directions. International Journal of Biomedical Research Science (IJBRS). 2026;02(1). Available from: <a href=”https://shorturl.at/4APKP“>https://shorturl.at/4APKP</a>
INTRODUCTION
Magnetic Resonance Imaging (MRI) is a cornerstone of modern diagnostic medicine, providing high-resolution images of internal body structures using non-ionizing electromagnetic fields [1-3]. Since its introduction in the 1980s [4], MRI has revolutionized the way medical professionals diagnose and monitor a wide range of conditions, from neurological disorders to cardiovascular diseases. The widespread use of MRI is due in large part to its ability to offer detailed anatomical and functional information without the risks associated with ionizing radiation, such as that used in X-rays and CT scans. This has established MRI as a preferred modality in many clinical and research settings [5-8].
However, as MRI technology has advanced, so too have concerns regarding its long-term safety, particularly for healthcare workers who are regularly exposed to the powerful magnetic fields generated by MRI machines. While MRI is generally regarded as safe for patients due to the relatively short duration of exposure, the same may not hold true for medical staff, who may be exposed to these fields for hours each day over the course of their careers. These concerns have been amplified with the increasing use of high-field MRI systems, such as those operating at 3 Tesla (T) or higher, which offer greater image resolution and contrast but also produce stronger magnetic fields that could pose a greater risk of biological effects [9,10].
The potential biological effects of MRI exposure are associated with three primary sources: static magnetic fields, time-varying gradient magnetic fields, and RF fields [11]. Static magnetic fields, which are a constant feature of MRI, can interact with biological tissues, leading to effects such as magneto hydrodynamic phenomena, which can cause dizziness and other sensory disturbances [12,13]. Time-varying gradient magnetic fields are used to spatially encode the MRI signal and can induce electrical currents in the body, potentially leading to peripheral nerve stimulation. RF fields are responsible for heating tissues, and while regulations limit the specific absorption rate (SAR) to prevent excessive heating, higher field strengths could pose a greater risk of localized tissue damage [14].
A key concern for healthcare workers is the cumulative effect of prolonged exposure to these fields over time. While individual MRI examinations may not pose a significant risk, repeated exposure over months or years could potentially lead to adverse health outcomes. For example, studies have reported transient effects such as dizziness, vertigo, metallic taste, and concentration difficulties among MRI technicians and radiologists, suggesting that there may be physiological consequences to long-term occupational exposure to MRI environments [15-17].
To date, research on the long-term effects of MRI exposure has been inconclusive. Several studies have examined the acute effects of MRI exposure, often focusing on short-term symptoms such as dizziness or nausea. However, fewer studies have investigated the long-term health consequences for healthcare workers who are exposed to MRI environments on a regular basis. Existing studies are often limited by small sample sizes, short follow-up periods, or a lack of consistent exposure measurement. Additionally, there is significant variability in the levels of exposure experienced by MRI staff, depending on factors such as their proximity to the MRI machine, the duration of exposure, and the strength of the magnetic field. [18-23]
Despite the growing body of research, many questions remain unanswered. For instance, it is unclear whether chronic exposure to high-field MRI could lead to more serious health conditions, such as cognitive impairment, cardiovascular issues, or even cancer. Additionally, the variability in exposure levels among MRI staff highlights the need for more precise monitoring and risk assessment protocols. Understanding the mechanisms by which MRI exposure might affect biological tissues is crucial for developing effective safety guidelines and minimizing risks for healthcare workers.
Given the increasing reliance on high-field MRI in both clinical and research settings, it is critical to assess the safety of long-term exposure to MRI environments, particularly for healthcare professionals who may be at higher risk. This study aims to provide a comprehensive review of the current literature on the biological effects of MRI exposure, with a particular focus on healthcare workers who are regularly exposed to high-field MRI. By synthesizing existing research, this review will identify both the potential benefits and risks associated with long-term MRI exposure, and will highlight areas where further research is needed to fill existing knowledge gaps. The outome of this review will contribute to the development of more robust safety guidelines for healthcare workers, ensuring that the benefits of MRI technology can be fully realized without compromising the health and safety of those who operate these systems daily. Furthermore, by identifying gaps in the current literature, this study will help to inform future research priorities and guide the development of new safety protocols for high-field MRI environments.
MATERIALS AND METHODS
Figure 1 illustrates a flow chart describing that A comprehensive review was conducted of the biological effects of MRI exposure by systematically searching relevant literature across multiple databases, including PubMed, Google Scholar, Scopus, and Science Direct, ensuring broad coverage of scientific publications and clinical studies .The search was performed using specific keywords and Boolean operators, such as “MRI exposure,” “biological effects of MRI,” “occupational health MRI staff,” “high-field MRI safety,” and “MRI-induced cognitive effects.” Boolean operators (e.g., AND, OR) were applied to refine and combine search terms where necessary. The complete list of all search terms and combinations used in this review is provided in Appendix A to facilitate reproducibility and to support future related research. The search spanned studies published between 2000 and 2024, focusing on research related to MRI machines operating at field strengths of 1.5 Tesla and above. This threshold was chosen because these field strengths are the most widely used in clinical environments and generate stronger magnetic fields, making them more relevant for evaluating occupational safety.
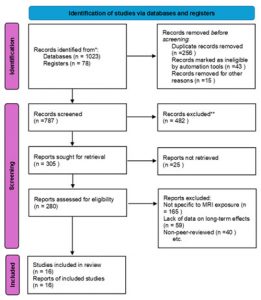
Figure 2 illustrates the study review criteria applied in this review, including both inclusion and exclusion parameters. Studies investigating biological effects on healthcare staff—such as MRI technicians, radiologists, and other medical professionals frequently exposed to MRI environments—were included. In addition to the database search, we conducted a manual review, which involved screening the reference lists of all included studies to identify additional relevant articles not captured during the initial search. These additional articles were retrieved, read in full, and assessed against the same inclusion and exclusion criteria to ensure eligibility. physiological changes, and potential long-term risks such as DNA damage. Studies that did not meet these criteria were excluded from the review.

RESULTS
The analysis of studies [24–39] on magnetic resonance imaging (MRI) exposure reveals both immediate and potential long-term health effects for individuals in MRI environments. Studies such as [24] identified short-term subjective symptoms (e.g., drowsiness, concentration issues) among healthcare professionals exposed to MRI. However, symptoms typically resolved within weeks, suggesting possible adaptation. Studies [25–28] explored the physiological impacts of ultra-high-field (UHF) MRI systems (≥7T), noting transient effects like dizziness and vertigo but insufficient evidence for lasting biological damage, underscoring the need for regular monitoring and strict adherence to occupational safety protocols.
For MRI technicians and workers in industries with static magnetic fields, studies [29,30] noted sleep disturbances and inconclusive cancer risks, emphasizing the need for improved exposure assessment and ongoing health monitoring. In particular, the lack of conclusive epidemiological studies limits understanding of MRI’s cumulative effects over extended periods, especially at high field strengths. Studies focusing on childhood leukemia and environmental EMF exposure, such as studies [31–39], present conflicting findings. While some meta-analyses [35,39] indicate a potential link between extremely low-frequency (ELF) magnetic fields (≥0.4 µT) and childhood leukemia, others report no definitive associations, suggesting that results may vary by exposure intensity and environmental factors. These discrepancies highlight the necessity for further large-scale, longitudinal studies to clarify long-term EMF impacts, particularly among children and other vulnerable groups.
DISCUSSION
This review highlights the current understanding and gaps in knowledge regarding the health impacts of MRI and EMF exposure. Short-term symptoms like dizziness, concentration issues, and drowsiness are frequently reported by healthcare workers in MRI environments, with most symptoms resolving over time. However, there remains limited and inconclusive data on the long-term effects of high-field MRI and EMF exposure, particularly concerning cumulative health risks such as cancer, reproductive effects, and neurological impacts. Notably, studies focusing on extremely low-frequency (ELF) magnetic fields in residential settings indicate a potential association with an increased risk of childhood leukemia, though findings vary across studies and depend on factors such as exposure intensity and environmental context. The lack of definitive evidence on long-term effects points to an urgent need for more rigorous epidemiological studies, particularly longitudinal research that examines cumulative exposure in both occupational and residential contexts.
For healthcare professionals, especially MRI technicians and radiologists, the growing use of ultra-high-field (≥7T) MRI technology warrants strict adherence to occupational safety protocols, including regular monitoring and exposure assessments. Furthermore, the potential vulnerability of children and other high-risk groups to prolonged EMF exposure emphasizes the need for precautionary measures in both clinical and residential environments. Considering these findings, developing robust, evidence-based guidelines for MRI and EMF safety is essential to balance the benefits of MRI technology with the health and safety of both patients and healthcare workers. Future research should prioritize understanding the biological mechanisms behind EMF-related health effects and evaluating the long-term impacts on diverse populations to establish clear and actionable safety standards. This study underscores the necessity of proactive safety protocols and continued research to support the safe and effective use of MRI in healthcare settings.
CONCLUSION
This review highlights the current understanding and remaining gaps regarding the health impacts of MRI and EMF exposure in occupational settings. Short-term effects such as dizziness, vertigo, and concentration difficulties are commonly reported but generally resolved over time, while evidence for long-term risks remains limited and inconclusive. The growing use of ultra-high-field MRI underscores the need for rigorous exposure monitoring, standardized safety protocols, and targeted research particularly large-scale longitudinal studies to clarify potential cumulative effects. For now, strict adherence to occupational safety measures remains the most effective strategy to protect MRI staff and patients while enabling the continued safe use of MRI technology.
REFERENCES
- Al Khudairi, O. A., Alasiri, R. S. A., Al Saiary, S. O. S., Al-Shalail, G. A., Hadi, S. M. A., Alyami, S. H. H., & Al Shreeh, N. H. (2023). Radiation In Diagnostic Imaging: An In-Depth Examination. Journal of Survey in Fisheries Sciences, 10(5), 118-124.
- Spagnuolo, G., & Soltani, P. (2024). Magnetic Resonance Imaging in digital dentistry: The start of a new era. Prosthesis, 6(4), 798-802.
- Ibrayeva, L., Grebeneva, O., Shadetova, A., Rybalkina, D., Minbayeva, L., Bacheva, I., & Alekseyev, A. (2021). Effect of non-ionizing radiation on the health of medical staff of magnetic resonance imaging rooms. Journal of clinical medicine of Kazakhstan, 18(4), 16-22.
- Blamire, A. M. (2008). The technology of MRI—the next 10 years? The British journal of radiology, 81(968), 601-617.
- Aljahdali, S., Azim, G., Zabani, W., Bafaraj, S., Alyami, J., & Abduljabbar, A. (2024). Effectiveness of radiology modalities in diagnosing and characterizing brain disorders. Neurosciences Journal, 29(1), 37-43.
- Hussain, S., Mubeen, I., Ullah, N., Shah, S. S. U. D., Khan, B. A., Zahoor, M., … & Sultan, M. A. (2022). Modern diagnostic imaging technique applications and risk factors in the medical field: a review. BioMed research international, 2022(1), 5164970.
- Ashby, K., Adams, B. N., & Shetty, M. (2020). Appropriate magnetic resonance imaging ordering.
- Ghadimi, M., & Sapra, A. (2019). Magnetic resonance imaging contraindications.
- Hartwig, V., Giovannetti, G., Vanello, N., Lombardi, M., Landini, L., & Simi, S. (2009). Biological effects and safety in magnetic resonance imaging: a review. International journal of environmental research and public health, 6(6), 1778-1798.
- Mittendorff, L., Young, A., & Sim, J. (2022). A narrative review of current and emerging MRI safety issues: What every MRI technologist (radiographer) needs to know. Journal of medical radiation sciences, 69(2), 250-260.
- Formica, D., & Silvestri, S. (2004). Biological effects of exposure to magnetic resonance imaging: an overview. Biomedical engineering online, 3, 1-12.
- Schenck, J. F. (2005). Physical interactions of static magnetic fields with living tissues. Progress in biophysics and molecular biology, 87(2-3), 185-204.
- Kangarlu, A., & Robitaille, P. M. L. (2000). Biological effects and health implications in magnetic resonance imaging. Concepts in Magnetic Resonance: An Educational Journal, 12(5), 321-359.
- Sammet, S. (2016). Magnetic resonance safety. Abdominal radiology, 41, 444-451.
- Glans, A., Wilén, J., Lindgren, L., Björkman-Burtscher, I. M., & Hansson, B. (2022). Health effects related to exposure of static magnetic fields and acoustic noise—comparison between MR and CT radiographers. European Radiology, 32(11), 7896-7909.
- Grant, A., Metzger, G. J., Van de Moortele, P. F., Adriany, G., Olman, C., Zhang, L., … & Uğurbil, K. (2020). 10.5 T MRI static field effects on human cognitive, vestibular, and physiological function. Magnetic resonance imaging, 73, 163-176.
- Cavin, I. D., Glover, P. M., Bowtell, R. W., & Gowland, P. A. (2007). Thresholds for perceiving metallic taste at high magnetic field. Journal of Magnetic Resonance Imaging: An Official Journal of the International Society for Magnetic Resonance in Medicine, 26(5), 1357-1361.
- Heinrich, A., Szostek, A., Meyer, P., Reinhard, I., Gilles, M., Paslakis, G., … & Nees, F. (2014). Women are more strongly affected by dizziness in static magnetic fields of magnetic resonance imaging scanners. Neuroreport, 25(14), 1081-1084.
- Saito, N., Hirano, T., & Kuwatsuru, R. (2024). Risk factors for imaging abnormalities in patients with dizziness complaints: an algorithm for ordering brain imaging. Clinical Radiology.
- Kabra, R., Robbie, H., & Connor, S. E. J. (2015). Diagnostic yield and impact of MRI for acute ischaemic stroke in patients presenting with dizziness and vertigo. Clinical Radiology, 70(7), 736-742.
- Saber Tehrani, A. S., Kattah, J. C., Mantokoudis, G., Pula, J. H., Nair, D., Blitz, A., … & Newman-Toker, D. E. (2014). Small strokes causing severe vertigo: frequency of false-negative MRIs and nonlacunar mechanisms. Neurology, 83(2), 169-173.
- Zanotti, G., Ligabue, G., & Gobba, F. (2015). Subjective symptoms and their evolution in a small group of magnetic resonance imaging (MRI) operators recently engaged. Electromagnetic Biology and Medicine, 34(3), 262-264.
- Touitou, Y., Djeridane, Y., Lambrozo, J., Camus, F., & Selmaoui, B. (2013). Long-term (up to 20 years) effects of 50-Hz magnetic field exposure on immune system and hematological parameters in healthy men. Clinical biochemistry, 46(1-2), 59-63.
- Zanotti, G., Ligabue, G., & Gobba, F. (2015). Subjective symptoms and their evolution in a small group of magnetic resonance imaging (MRI) operators recently engaged. Electromagnetic Biology and Medicine, 34(3), 262-264.
- Ladd, M. E., Bachert, P., Meyerspeer, M., Moser, E., Nagel, A. M., Norris, D. G., … & Zaiss, M. (2018). Pros and cons of ultra-high-field MRI/MRS for human application. Progress in nuclear magnetic resonance spectroscopy, 109, 1-50.
- Schenck, J. F. (2000). Safety of strong, static magnetic fields. Journal of magnetic resonance imaging, 12(1), 2-19.
- Expert Panel on MR Safety: Kanal, E., Barkovich, A. J., Bell, C., Borgstede, J. P., Bradley Jr, W. G., … & Hernandez, D. (2013). ACR guidance document on MR safe practices: 2013. Journal of Magnetic Resonance Imaging, 37(3), 501-530.
- Formica, D., & Silvestri, S. (2004). Biological effects of exposure to magnetic resonance imaging: an overview. Biomedical engineering online, 3, 1-12.
- Huss, A., Özdemir, E., Schaap, K., & Kromhout, H. (2021). Occupational exposure to MRI-related magnetic stray fields and sleep quality among MRI–Technicians-A cross-sectional study in the Netherlands. International Journal of Hygiene and Environmental Health, 231, 113636.
- Feychting, M. (2005). Health effects of static magnetic fields—a review of the epidemiological evidence. Progress in biophysics and molecular biology, 87(2-3), 241-246.
- Touitou, Y., Djeridane, Y., Lambrozo, J., Camus, F., & Selmaoui, B. (2013). Long-term (up to 20 years) effects of 50-Hz magnetic field exposure on immune system and hematological parameters in healthy men. Clinical biochemistry, 46(1-2), 59-63.
- National Research Council (US) Committee on the Possible Effects of Electromagnetic Fields on Biologic Systems. (1997). Possible health effects of exposure to residential electric and magnetic fields (Executive summary). National Academies Press. https://www.ncbi.nlm.nih.gov/books/NBK232727/
- Scientific Committee on Emerging Newly Identified Health Risks. (2015). Opinion on potential health effects of exposure to electromagnetic fields. Bioelectromagnetics, 36(6), 480-484.
- Moon, J. H. (2020). Health effects of electromagnetic fields on children. Clinical and experimental pediatrics, 63(11), 422.
- Schüz, J. (2011). Exposure to extremely low-frequency magnetic fields and the risk of childhood cancer: update of the epidemiological evidence. Progress in biophysics and molecular biology, 107(3), 339-342.
- Schüz, J., & Erdmann, F. (2016). Environmental exposure and risk of childhood leukemia: an overview. Archives of medical research, 47(8), 607-614.
- London, S. J., Thomas, D. C., Bowman, J. D., Sobel, E., Cheng, T. C., & Peters, J. M. (1991). Exposure to residential electric and magnetic fields and risk of childhood leukemia. American journal of epidemiology, 134(9), 923-937.
- Fatahi, M., Reddig, A., Friebe, B., Reinhold, D., & Speck, O. (2017). MRI and genetic damage: an update. Current Radiology Reports, 5, 1-7.
- Ghahremani, S., Shiroudbakhshi, K., Salimi Kordasiabi, A. H., FiroozBakht, M., Hosseinzadegan, M., Ashrafinia, F., & Rahafard, S. (2020). Exposure to magnetic fields and childhood leukemia: An overview of meta-analysis. International Journal of Pediatrics, 8(5), 11361-11365.



